5 Minutes
When a doctor says the words that change everything, the consequences can go far beyond scans and chemotherapy. Some people rearrange priorities; others confront depression, financial strain, or a new sense of mortality. A recent Danish study suggests another, less obvious consequence: a measurable rise in criminal convictions in the years after a cancer diagnosis.
At first glance, the pattern surprises. The study—an expansive administrative-data analysis covering 368,317 Danes diagnosed with cancer from 1980 to 2018—shows that crime actually dips in the first year after diagnosis. That makes sense. Intensive treatment schedules and the physical toll of therapy tend to keep patients away from settings where many offenses occur.
But two years out, the curve turns. Conviction rates climb above patients’ pre-diagnosis baseline, reach a peak around five years after diagnosis, and then level off at an elevated rate that persists for roughly another five years. Overall, the researchers estimate a roughly 14 percent higher likelihood of conviction compared with people who never received a cancer diagnosis.
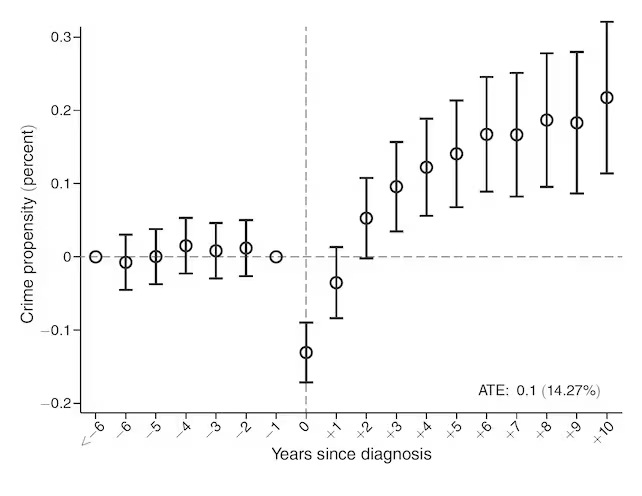
Effect of cancer on crime.
Methods and what the data reveal
The strength of the paper lies in data linkage: Denmark’s administrative registers let economists merge records for demographics, employment, income, health, and criminal history at the individual level. That makes it possible to follow each person before and after diagnosis and to compare them with a control group that did not receive a cancer diagnosis during the same period.
Design like this reduces some confounders. But natural experiments and subgroup checks are also required to move from correlation toward causation. The authors exploit variation caused by municipal reforms in 2007—places where social support was trimmed versus those where it was not—to test whether welfare buffers change the crime signal. They also split patients by estimated five-year survival probability (based on cancer type, age, sex, and marital status) to see whether expected longevity matters.
Two mechanisms stand out. First, economic decline. Even in a universal health-care system like Denmark’s, cancer often knocks people out of the labor force. Employment probability falls, hours and earnings drop, and those income shocks correlate with greater rates of property and drug-related crimes. Second, mortality expectations. Patients whose five-year survival probability drops sharply after diagnosis show a stronger link to later criminal convictions. The implication: when the future feels shorter, the deterrent power of long-term sanctions may weaken.
Not all offenses fit neatly into an economic explanation. The study reports rises in violent and non-economic crimes as well, indicating that psychological stress, substance misuse, social isolation, or disrupted support networks could play roles. In places where municipal social supports were reduced after the 2007 reform, the post-diagnosis crime increase was more pronounced—consistent with a social-safety-net effect.
Implications for policy and public health
What should clinicians, policymakers, and communities take from this? First: medical care alone is not the whole answer. Health shocks cascade into labor markets, household finance, and social networks. Some survivors will need employment accommodations, targeted income support, or mental-health and substance-use services to prevent downstream harms.
Second: research like this reframes how we think about prevention. Public health interventions that reduce the economic fallout of illness—job protection, disability benefits calibrated to income loss, or rapid re-employment programs—could also reduce crime indirectly. The study’s natural experiment suggests these levers matter.
Finally, translation matters. The paper is an economics study, but its audience spans clinicians, social workers, and criminal-justice professionals. That interdisciplinary reach is necessary when the consequences of a diagnosis radiate through health, work, and law.
Expert Insight
"The findings push us to view serious illness as a social shock, not just a medical one," says Dr. Lena Sørensen, a health economist at the University of Copenhagen. "When someone’s time horizon shortens or household income collapses, behavior can change in ways policymakers rarely anticipate. Strengthening targeted supports in the years after diagnosis could reduce both individual and societal harms."
She adds: "We must be careful in interpretation. This is robust evidence of a pattern, not a blanket statement about all cancer patients. Most people do not commit crimes. But the elevated risk for a subset is enough to justify policy attention."
Open questions remain. How do different cancer types and stages map to behavioral risk? Which psychosocial interventions are most protective? Can rehabilitation programs tailored to survivors reduce recidivism where offenses occur? The Danish registers provide clear signals; now the work moves toward targeted trials and cross-national replication. If other countries show similar patterns, the finding could reshape post-diagnosis care models and inform cross-sector strategies that blend public health, labor policy, and criminal-justice reform.
Researchers and practitioners are already asking whether existing survivorship programs reach those most at risk—and whether a modest investment in social buffering could avoid larger social costs later. If the evidence holds, treating the social and economic fallout of cancer might be as important as treating the tumor itself.
Source: sciencealert
Comments
Armin
Is this even causal? 14% higher seems vague, maybe a few groups drive it... Denmark's safety net is unique, unclear how this maps elsewhere, more breakdown pls
labcore
wow that hit me. didnt expect crime to rise years after diagnosis. social supports huge, ppl need help not blame

Leave a Comment