6 Minutes
Could a thin, overlooked organ tucked between mother and fetus carry the earliest warnings of serious mental illness? Evidence is mounting that the placenta—more than a passive filter—records chemical and genetic footprints of pregnancy that may foreshadow neurodevelopmental outcomes decades later.
Research and methods
Researchers at Western University set out to test a simple yet consequential question: does prenatal exposure to THC, the mind‑altering component of cannabis, alter placental signals already linked to schizophrenia? The motivation is clear. Schizophrenia affects about one percent of Canadians and shortens lives through a combination of psychiatric, social and physical health burdens. Early detection matters because interventions begun sooner tend to improve long‑term outcomes.
The team drew on two complementary experimental systems. First, pregnant rodents consumed a THC‑infused edible—yes, mixed with Nutella—mimicking an oral exposure route common in humans. Offspring were then tested for sensorimotor gating using prepulse inhibition, a behavioural assay that quantifies the brain’s ability to filter distraction; deficits on this test are a translational marker often associated with schizophrenia.
Short answer: offspring exposed in utero exhibited reduced prepulse inhibition early in life. More than behaviour, the investigators examined the placentas from these pregnancies and found increased expression of a set of placental genes that prior studies have tied to higher schizophrenia risk. In other words, THC changed both physiology and placental molecular patterns.
Human placental cells in culture
To bridge the gap between rodents and people, the researchers exposed isolated human placental cells to THC for 24 hours. The result echoed the animal work: several schizophrenia‑related genes rose in activity after short‑term THC exposure. While cell cultures cannot capture the full complexity of a pregnancy, they offer direct evidence that human placental tissue responds to THC in ways that mirror the rodent findings.
Context and significance
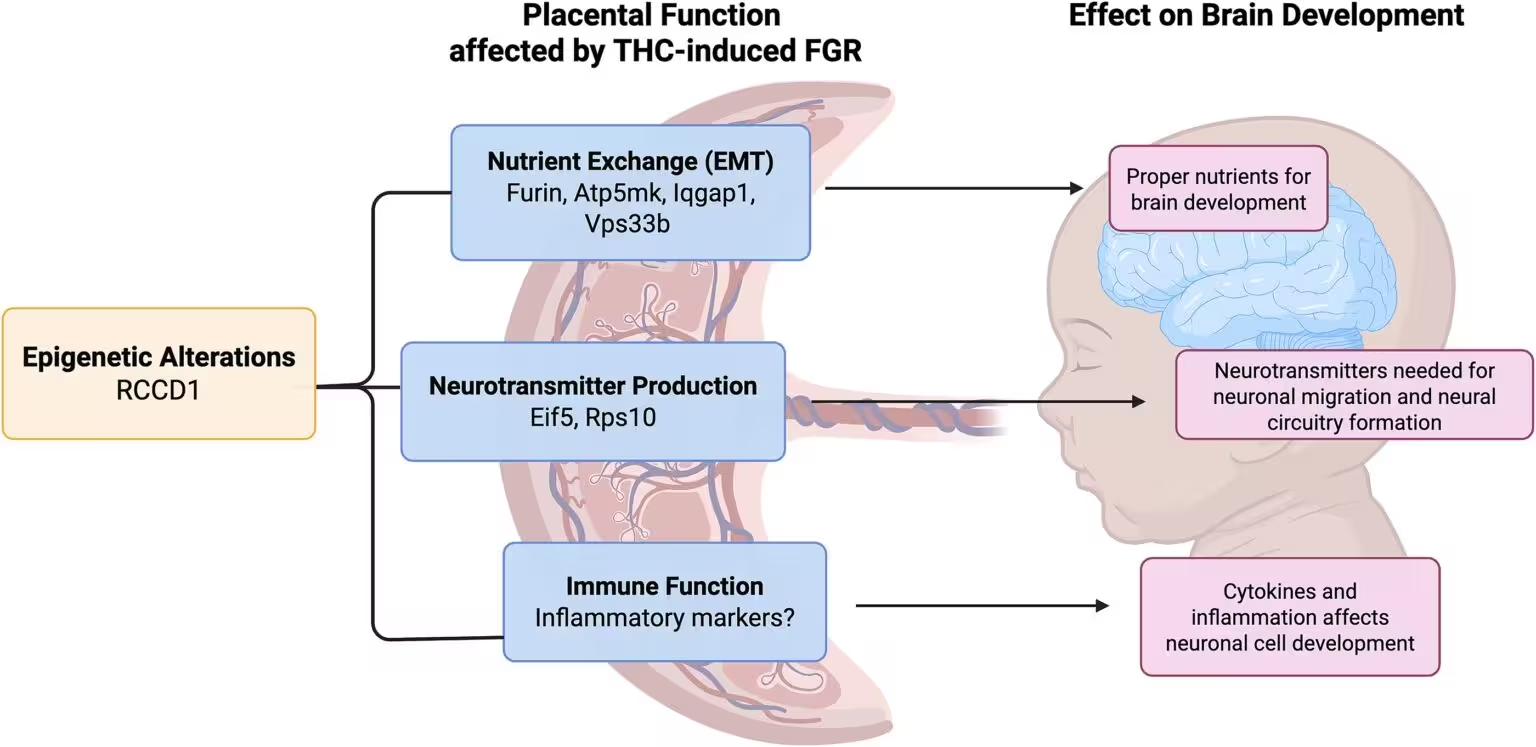
The notion that the placenta and brain are linked is not new: the placenta‑brain axis describes how placental health influences fetal brain development via nutrient delivery, hormonal signals and immune modulation. Large cohort studies have already shown altered placental markers in pregnancies with low birth weight—a known correlate of later neuropsychiatric conditions, including schizophrenia and autism.
What changes here is specificity. The Western University study suggests that prenatal cannabis exposure does not merely raise the odds of low birth weight; it may selectively perturb placental genes implicated in schizophrenia pathways. That distinction matters for screening. If placentas can be tested at birth for a THC‑associated molecular signature, clinicians could identify infants at elevated neurodevelopmental risk long before psychiatric symptoms emerge—years before typical schizophrenia onset between late adolescence and early adulthood.
Policy and public health implications are immediate. Cannabis legalization in Canada in 2018 coincided with rising prenatal use, particularly among adolescents, where reported rates reached nearly one quarter. Stopping cannabis during pregnancy is the safest medical advice, yet real barriers exist: dependence, social factors and lack of counseling resources. A placental test would not remove the need for prevention, but it could channel early supports—behavioral therapy, nutritional interventions, close developmental monitoring—to children most likely to benefit.
Implications and open questions
Several crucial unknowns remain. Does cannabidiol (CBD), another abundant cannabinoid often perceived as benign, alter the same placental markers? What about paternal cannabis use before conception—can sperm‑borne changes influence the placenta indirectly? The current study hints at mechanistic links but cannot prove causation for human psychiatric diagnoses decades after birth. Longitudinal birth cohorts that combine placental molecular profiling with detailed exposure histories and follow‑up into adolescence will be necessary.
There is also the matter of specificity. Are the THC‑linked placental signatures unique to schizophrenia risk, or do they predict a wider range of neurodevelopmental outcomes such as autism spectrum conditions or cognitive impairment? Early evidence suggests overlap; placental stressors often map to multiple behavioural trajectories depending on timing, dose and genetic vulnerability.
Expert Insight
"The placenta is a living archive of pregnancy exposures," says Dr. Miriam Cole, a perinatal neuroscientist not involved in the study. "What this work does is give us a plausible molecular thread connecting cannabis exposure to later brain function. It doesn’t close the loop—no single study can—but it opens a testable path toward early identification and, eventually, intervention."
"From a clinical standpoint," adds Dr. Cole, "a validated placental screen could transform follow‑up care. Imagine pediatric teams alerted at birth to a specific risk profile and able to offer focused developmental support rather than waiting until a child struggles in school or adolescence."
The findings provide functional data for clinicians and regulators as they weigh the safety of cannabis use in pregnancy. They also underscore practical next steps: replication in humans, evaluation of CBD and other cannabinoids, and development of standardized placental assays that could be integrated into perinatal practice.
For now, the message to expectant parents is cautious: cannabis exposure during pregnancy can change placental biology in ways linked to altered brain development. The placenta may not only nourish life; it may also whisper warnings about risks yet to unfold.
Source: sciencealert
Comments
Tomas
is this even true? Rodent effects are one thing, 24h in cell culture another. How do they leap to decades of risk... curious, but pretty skeptical
bioNix
wow, placenta as a record? kinda chilling. If THC leaves a fingerprint at birth, that could change follow up care... but we need cohorts, not just Nutella rats


Leave a Comment