5 Minutes
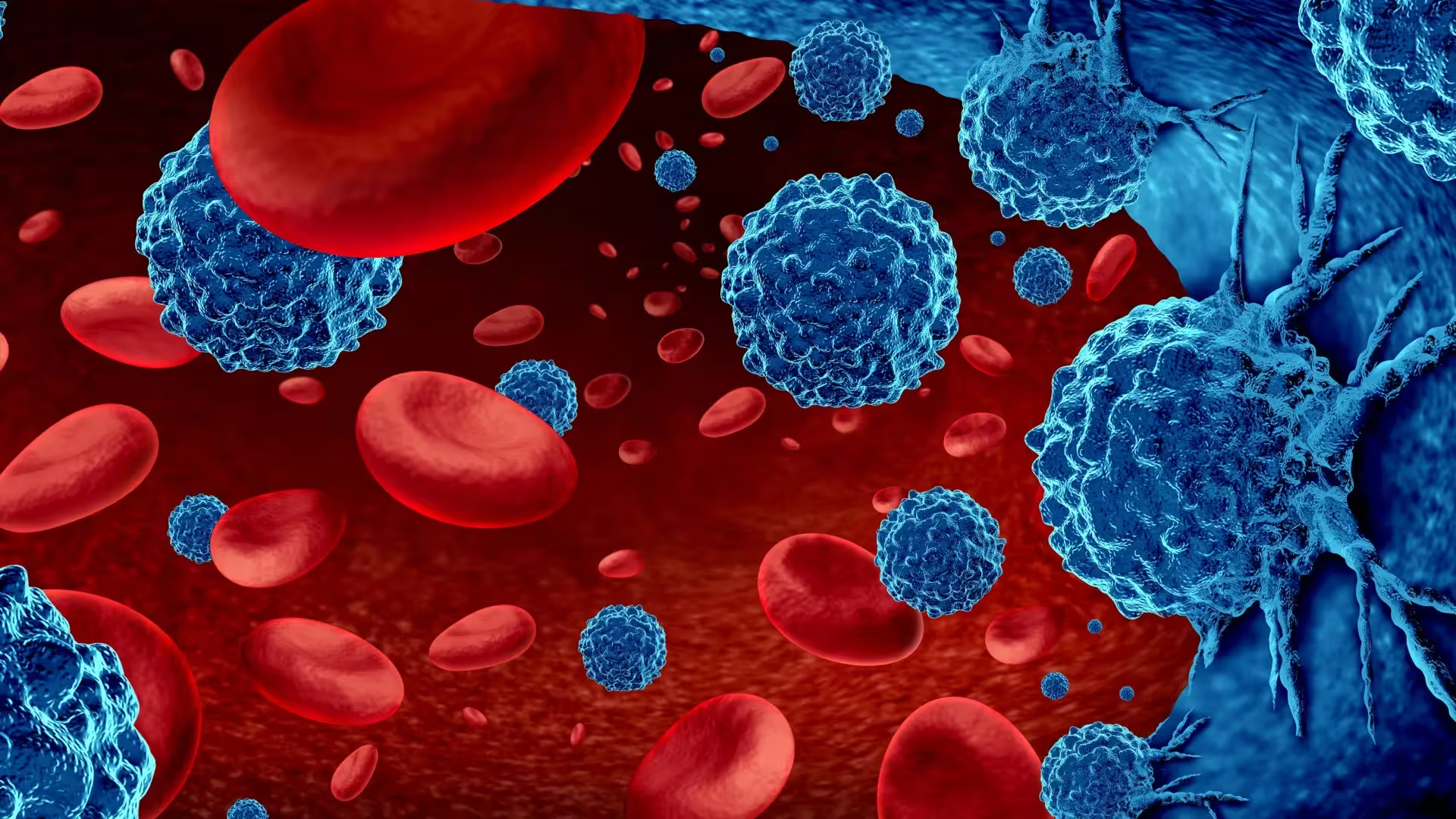
Cutting off blood flow to tissues can prematurely age the bone marrow and shift the immune system into a cancer-tolerant state, according to a new study from NYU Langone Health published in JACC: CardioOncology. In mouse models of breast cancer, temporary ischemia in a hind limb doubled tumor growth compared with mice that had normal blood flow. The experiments indicate that peripheral ischemia — the reduced oxygen delivery caused by blocked arteries in the legs — reprograms bone marrow stem cells and skews immune cell production toward populations that suppress, rather than attack, tumors. Image credit: Shutterstock
Scientific background: ischemia, peripheral artery disease and cancer risk
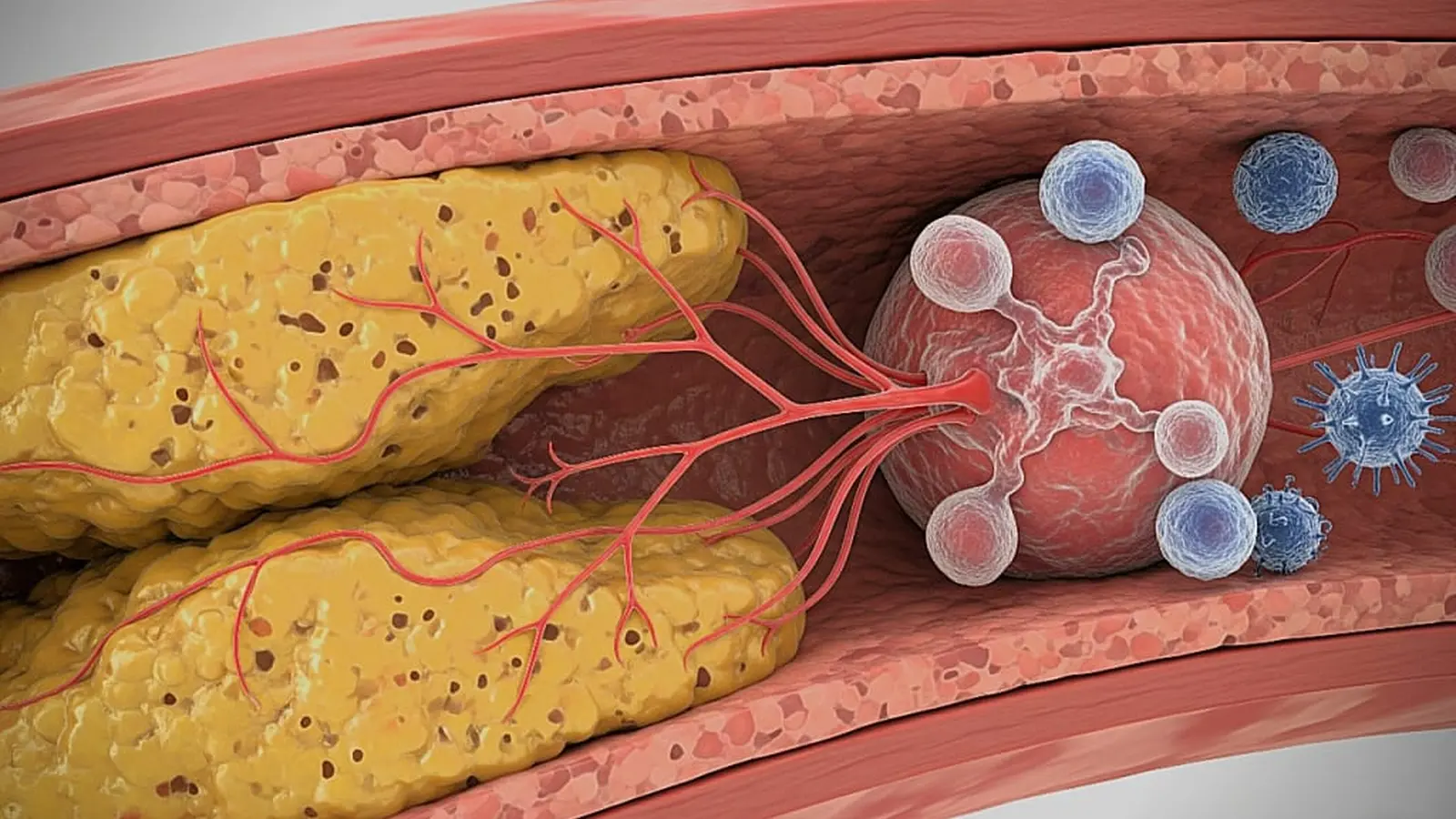
Ischemia arises when fat, cholesterol and inflammation narrow arteries and limit the delivery of oxygen-rich blood. In the legs, this condition is known as peripheral artery disease (PAD), which affects millions worldwide and raises the risk of heart attack and stroke. NYU researchers expanded on prior work (including a 2020 study linking heart-attack–related ischemia to faster tumor growth) to test how ischemia outside the heart influences systemic immunity and cancer progression.
The immune system relies on bone marrow stem cells to replace and supply white blood cells throughout life. With normal blood flow, the system balances inflammatory responses (to clear infections or damaged tissue) with regulatory signals that limit collateral damage. The NYU study shows that ischemia perturbs that balance by altering stem cell programming in the marrow.
Methods and key findings
The team used a controlled mouse model carrying breast tumors and induced temporary ischemia in one hind limb to simulate PAD. They compared tumor progression, immune cell profiles, and gene regulation between ischemic and control animals.
Key findings:
- Tumor growth doubled in mice with limb ischemia versus controls.
- Bone marrow stem cells were reprogrammed to favor myeloid-lineage cells (monocytes, macrophages, neutrophils) that are associated with immune suppression.
- Production of lymphocytes, notably T cells that mediate anti-tumor immunity, was reduced.
- Tumor microenvironments accumulated immune-suppressive populations, including Ly6Chi monocytes, M2-like F4/80+ MHCIIlo macrophages, and regulatory T cells (Tregs).
- Ischemia led to durable changes in hundreds of genes and remodeled chromatin structure in immune cells, making it harder for anti-cancer programs to be activated.
Mechanism: bone marrow aging and immune skewing
The authors report that ischemia effectively induces a premature aging phenotype in the bone marrow. Chromatin reorganization and altered gene expression transformed stem-cell output, producing a systemic immune landscape that tolerates tumor growth. As corresponding author Kathryn J. Moore, PhD, states, "Our study shows that impaired blood flow drives cancer growth regardless of where it happens in the body. This link between peripheral artery disease and breast cancer growth underscores the critical importance of addressing metabolic and vascular risk factors as part of a comprehensive cancer treatment strategy."
Long-term immune reprogramming
Beyond transient inflammation, ischemia produced long-lasting epigenetic and transcriptional shifts. These durable changes explain why a localized vascular event can remodel systemic immunity and create a permissive environment for cancer progression.
Clinical implications and future directions
This work suggests several translational paths: earlier cancer screening for patients with PAD, clinical trials testing whether inflammation-modulating or epigenetic therapies can reverse ischemia-driven immune changes, and integrated care strategies that target both vascular health and cancer risk. First author Alexandra Newman, PhD, notes, "These findings open the door to new strategies in cancer prevention and treatment, like earlier cancer screening for patients with peripheral artery disease and using inflammation-modulating therapies to counter these effects."
Next steps
The NYU team plans to support clinical studies assessing whether approved anti-inflammatory drugs or agents that modify chromatin accessibility can restore anti-tumor immunity after ischemic episodes.
Expert Insight
Dr. Elena Sánchez, an immuno-oncology researcher (fictional expert for context), comments: "The study elegantly connects vascular pathology to systemic immune aging. If similar mechanisms operate in humans, screening for cancer risk in patients with PAD could become an important preventive measure. It also points to treating inflammation and vascular disease as strategies to support immune surveillance."
Conclusion
NYU Langone's study provides mechanistic evidence that blocked blood flow outside the tumor — such as in peripheral artery disease — can accelerate cancer by reprogramming bone marrow stem cells and promoting immune-suppressive cell populations. These results link vascular health to cancer progression, highlighting the value of integrated cardiovascular and oncologic care, earlier screening for at-risk patients, and exploration of therapies that target inflammation and epigenetic changes to restore robust anti-tumor immunity.
Source: sciencedaily

Leave a Comment