4 Minutes
New Veterans Affairs study links nicotinamide to lower skin cancer recurrence
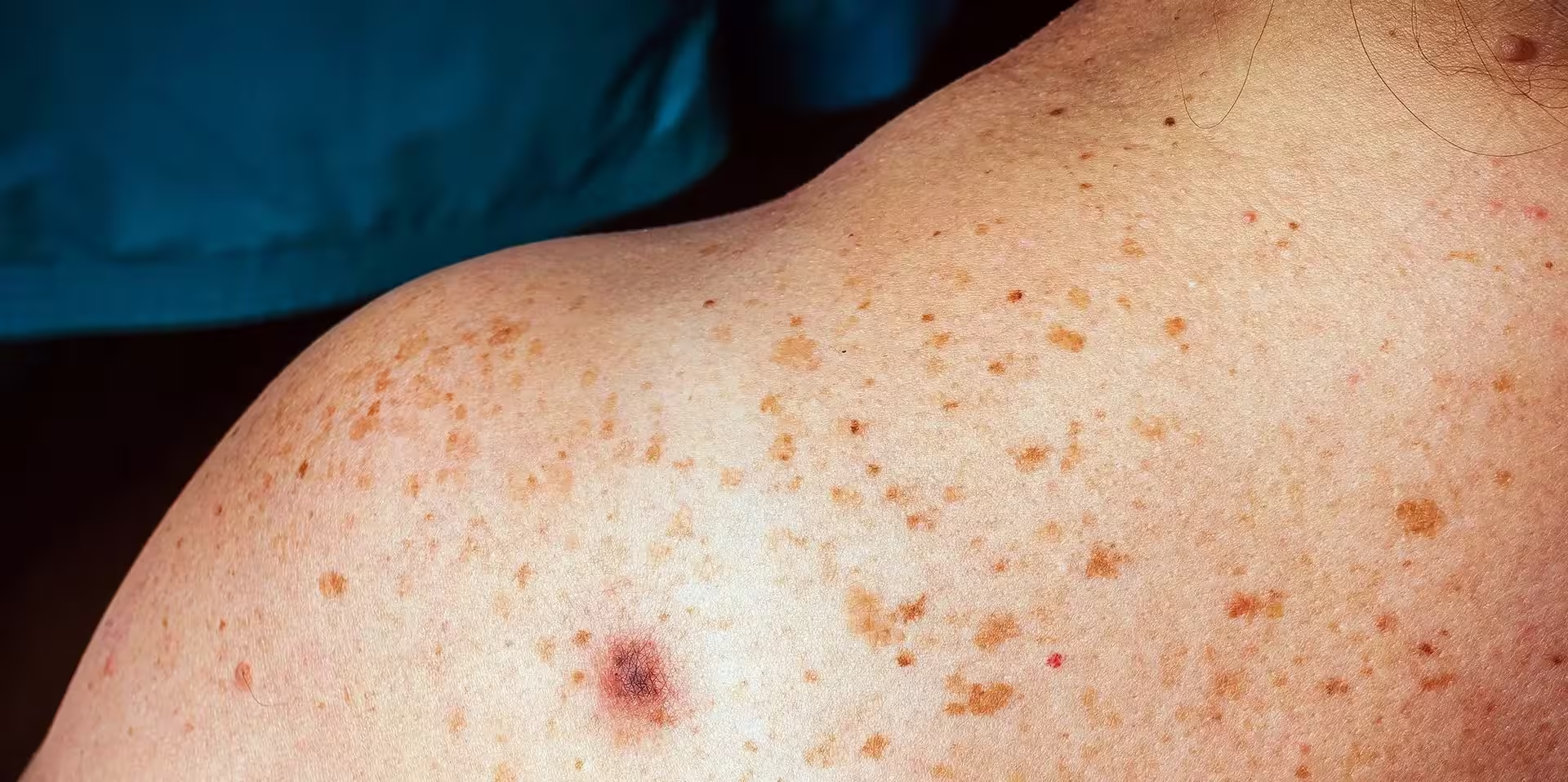
A large retrospective analysis of Veterans Affairs (VA) medical records indicates that nicotinamide—the over‑the‑counter form of vitamin B3—may reduce the risk of subsequent nonmelanoma skin cancers. Researchers examined outcomes for 33,833 patients and report the results in the Sept. 17 issue of JAMA Dermatology.
Dermatologists first began recommending nicotinamide for patients with prior skin cancer after a 2015 randomized trial of 386 participants showed fewer new lesions among supplement users. Because nicotinamide is widely available without a prescription, prior population-level follow-up has been scarce: use is often not recorded in routine medical charts. Investigators overcame this limitation by using the VA Corporate Data Warehouse, where nicotinamide appears in the VA formulary and dispensing records.
Study design and key findings
Investigators identified 33,833 patients who started a baseline nicotinamide regimen (500 mg twice daily for more than 30 days) and compared outcomes to 21,479 contemporaneous VA patients who did not receive the drug. The analysis targeted two common nonmelanoma skin cancers: basal cell carcinoma (BCC) and cutaneous squamous cell carcinoma (cSCC).
Overall, nicotinamide use was associated with a 14% reduction in the risk of developing another skin cancer. The effect was most pronounced when nicotinamide was started after a first skin cancer, with a 54% relative reduction in recurrence risk. Benefits diminished when treatment was initiated after multiple prior skin cancers. The protective signal was stronger for cutaneous squamous cell carcinoma than for basal cell carcinoma.
Corresponding author, Lee Wheless, MD, PhD, assistant professor of Dermatology and Medicine at Vanderbilt University Medical Center and a staff physician at VA Tennessee Valley Healthcare System. Credit: Vanderbilt University Medical Center
Immunocompromised and transplant subgroups
The team also examined 1,334 solid organ transplant recipients, a group at elevated risk for cSCC because of chronic immunosuppression. In this subgroup there was no significant overall reduction in new skin cancers, though early initiation of nicotinamide correlated with fewer squamous cell lesions in some analyses. The authors note that larger targeted trials in transplant recipients are still needed to confirm benefit.
Scientific context and clinical implications
Nicotinamide is a form of vitamin B3 involved in cellular metabolism and DNA repair pathways. Laboratory and small clinical studies have suggested it can reduce ultraviolet‑induced immunosuppression and support keratinocyte DNA repair after sun exposure—mechanisms consistent with an effect on nonmelanoma skin cancers.
These VA data strengthen the evidence base because they reflect a broader, real‑world population and long follow‑up. The study suggests dermatologists should consider earlier prophylactic use of nicotinamide—potentially after the first diagnosed skin cancer—rather than reserving it for patients with many prior lesions. However, clinicians must weigh individual risk factors, concurrent medications, and the limited signal in immunosuppressed patients.
Implications for research and practice
Key next steps include prospective trials in higher‑risk groups (for example, organ transplant recipients), investigation of optimal dosing and duration, and development of clinical guidelines to identify who is most likely to benefit. Because nicotinamide is well tolerated at common doses (500 mg twice daily) and inexpensive, it represents an accessible adjunct to sun protection and regular dermatologic surveillance.
Conclusion
This large VA study reinforces earlier trial data that nicotinamide can reduce the risk of subsequent nonmelanoma skin cancers, especially when started early after an initial diagnosis. While not a substitute for sun protection or dermatologic follow‑up, nicotinamide may be a low‑cost, low‑risk tool to help prevent additional basal cell and squamous cell carcinomas. Clinicians should discuss individual risks and benefits with patients and await further targeted studies in immunocompromised populations.
Source: scitechdaily

Leave a Comment