5 Minutes
Infection as a Trigger for Myocardial Infarction
Heart attacks may be initiated by dormant bacterial communities embedded in arterial plaques, new research suggests. Scientists report that cholesterol-rich atherosclerotic plaques can harbour jelly-like bacterial biofilms that remain asymptomatic for years, protected from both immune responses and antibiotics. A later viral infection or other systemic trigger can reactivate these biofilms, provoking local inflammation that weakens the plaque’s fibrous cap, promotes clot formation and can precipitate myocardial infarction.
Recent analyses used advanced molecular and histological methods to identify bacterial DNA and intact biofilm structures inside coronary and peripheral artery plaques. The presence of oral bacteria genetic material within atherosclerotic tissue provides direct evidence linking microbial communities to coronary artery disease — an association previously suspected but difficult to prove.
How Biofilms Operate and Break Dormancy
Biofilms are structured, surface-attached bacterial communities embedded in an extracellular matrix. That matrix acts as a barrier, reducing the effectiveness of antibiotics and concealing bacteria from immune cells. In the context of atherosclerosis, researchers found biofilm material lining cholesterol-rich plaques. When an external factor such as a viral infection stimulates the local environment, bacteria within the biofilm can resume growth and disperse, triggering a cascade of immune activation.
From inflammation to plaque rupture
Activated bacteria stimulate an inflammatory response that can degrade the collagen-rich fibrous cap covering a plaque. Degradation and thinning of this cap increases the risk of rupture; when a plaque ruptures, exposed plaque contents rapidly form a clot (thrombus) that can occlude a coronary artery and cause a heart attack.
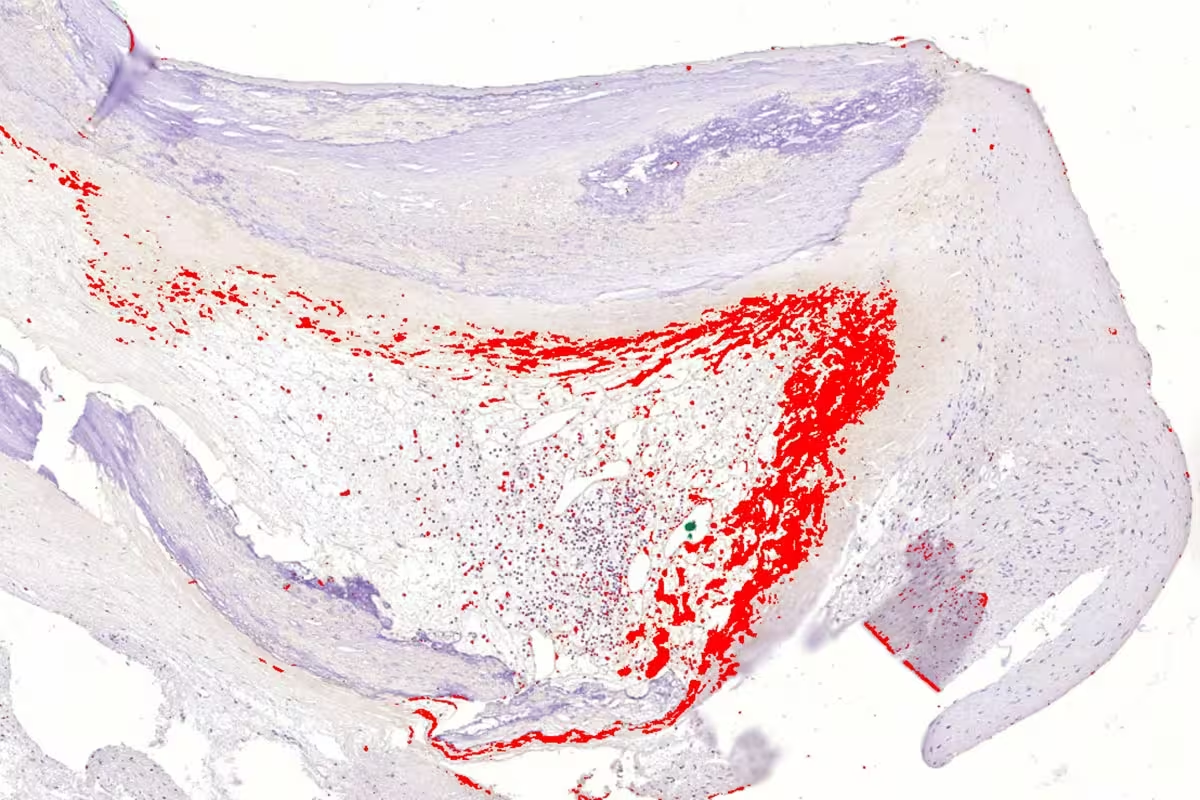
Asymptomatic bacterial biofilm lining a cholesterol-laden coronary artery plaque. Credit: Pekka Karhunen’s research group, Tampere University
Professor Pekka Karhunen, lead author of the study, notes that the field has long emphasized oxidised low-density lipoprotein (LDL) as a central driver of atherosclerosis. "Bacterial involvement in coronary artery disease has long been suspected, but direct and convincing evidence has been lacking. Our study demonstrated the presence of genetic material – DNA – from several oral bacteria inside atherosclerotic plaques," Karhunen says. The study team also developed an antibody targeted at these bacteria, which unexpectedly revealed visible biofilm structures in arterial tissue.
Study Scope, Methods and Collaborations
The study combined tissue analysis from multiple sources: samples from individuals who died of sudden cardiac death and samples from patients undergoing carotid and peripheral artery surgery. Institutions involved include Tampere University, Oulu University, the Finnish Institute for Health and Welfare and the University of Oxford. The work is part of an EU-funded cardiovascular research consortium spanning 11 countries, with additional funding from the Finnish Foundation for Cardiovascular Research and the Jane and Aatos Erkko Foundation.
Molecular detection of bacterial DNA, immunohistochemistry using newly developed antibodies, and visualization of biofilm structures gave the team convergent lines of evidence linking intra-plaque bacteria with cases of myocardial infarction.
Toward Diagnostics, Therapies and Vaccines
These findings open new avenues for diagnostics and preventive strategies. Targeted antibodies that detect intra-arterial biofilms could improve risk stratification for patients with atherosclerosis. More ambitiously, vaccination against specific oral or biofilm-forming bacteria could reduce the incidence of plaque activation and subsequent heart attacks, if future trials confirm causal benefit.
Antibiotics alone are unlikely to clear established biofilms because the extracellular matrix restricts drug penetration and many bacteria enter low-metabolic states. Novel therapies may combine biofilm-disrupting agents, immunomodulation and vaccination to prevent biofilm activation or enhance clearance.
Expert Insight
Dr. Sofia Nieminen, a fictional clinical microbiologist and cardiovascular researcher, comments: "This study reframes part of atherosclerosis as a chronic, infection-associated process in some patients. If replicated in larger cohorts, it would justify developing vaccines or targeted immune therapies to neutralize plaque-resident microbes. Translating this into clinical practice will require careful trials to prove that eliminating or neutralizing these bacteria lowers heart-attack risk without unintended consequences."
Conclusion
The discovery of bacterial biofilms inside atherosclerotic plaques strengthens the hypothesis that infectious agents can precipitate myocardial infarction by inducing local inflammation and plaque rupture. The research highlights new diagnostic biomarkers and suggests vaccination or anti-biofilm strategies as potential preventive tools. Ongoing multinational efforts will be needed to validate causal links and to move from molecular discovery to clinical interventions that could reduce heart-attack incidence worldwide.
Source: scitechdaily

Leave a Comment