6 Minutes
Movement, not pills: reframing osteoarthritis care
Stiff knees, sore hips and the grinding discomfort of chronic joint disease are often treated as inevitable consequences of aging. Yet emerging evidence and clinical reviews indicate that our approach to preventing and managing osteoarthritis is misaligned with what actually works. The most effective and accessible therapy for most people is not a medication or an operation but structured movement: targeted exercise and physiotherapy.
Across diverse health systems, from Ireland and the UK to Norway and the United States, fewer than half of patients diagnosed with osteoarthritis receive a formal referral to exercise-based care or physiotherapy from their primary provider. Instead, many are prescribed treatments that clinical guidelines discourage, and up to 40% are referred for surgical consultation before conservative measures have been fully explored.
Why exercise protects joints: the biology in brief
Osteoarthritis is the world’s most common joint disorder, already affecting hundreds of millions of people and projected to increase substantially by mid-century due to population aging, sedentary lifestyles and rising rates of overweight and obesity. Understanding what exercise does at a tissue and molecular level helps explain why it is so effective.
Cartilage — the resilient tissue that cushions bone ends — has no direct blood supply. It relies on cyclical mechanical loading to move fluid, nutrients and natural lubricants in and out of the matrix, much like squeezing and releasing a sponge. Regular movement maintains cartilage nutrition and surface integrity; prolonged inactivity reduces fluid exchange and impedes repair.
Because osteoarthritis involves not just cartilage but the whole joint environment — synovial fluid, subchondral bone, ligaments, surrounding muscle and the neural pathways that control movement — therapies that address multiple elements simultaneously are most useful. Exercise does that: it strengthens muscles that stabilise joints, improves neuromuscular control, reduces pro-inflammatory circulating factors and supports healthier metabolic profiles.
Exercise modalities that work
Therapeutic exercise for osteoarthritis includes strength (resistance) training, aerobic conditioning, flexibility work and neuromuscular training that targets balance and movement quality. Resistance training rebuilds muscle mass and joint support; aerobic activity improves cardiovascular health and reduces systemic inflammation.
Neuromuscular programs such as GLA:D® (Good Life with osteoArthritis: Denmark) combine supervised group sessions led by physiotherapists with education and practical movement training. These programs emphasise movement quality, balance and gradual load progression to restore joint stability and confidence. Multiple studies document clinically meaningful reductions in pain and improvements in function and quality of life lasting up to a year after program completion.

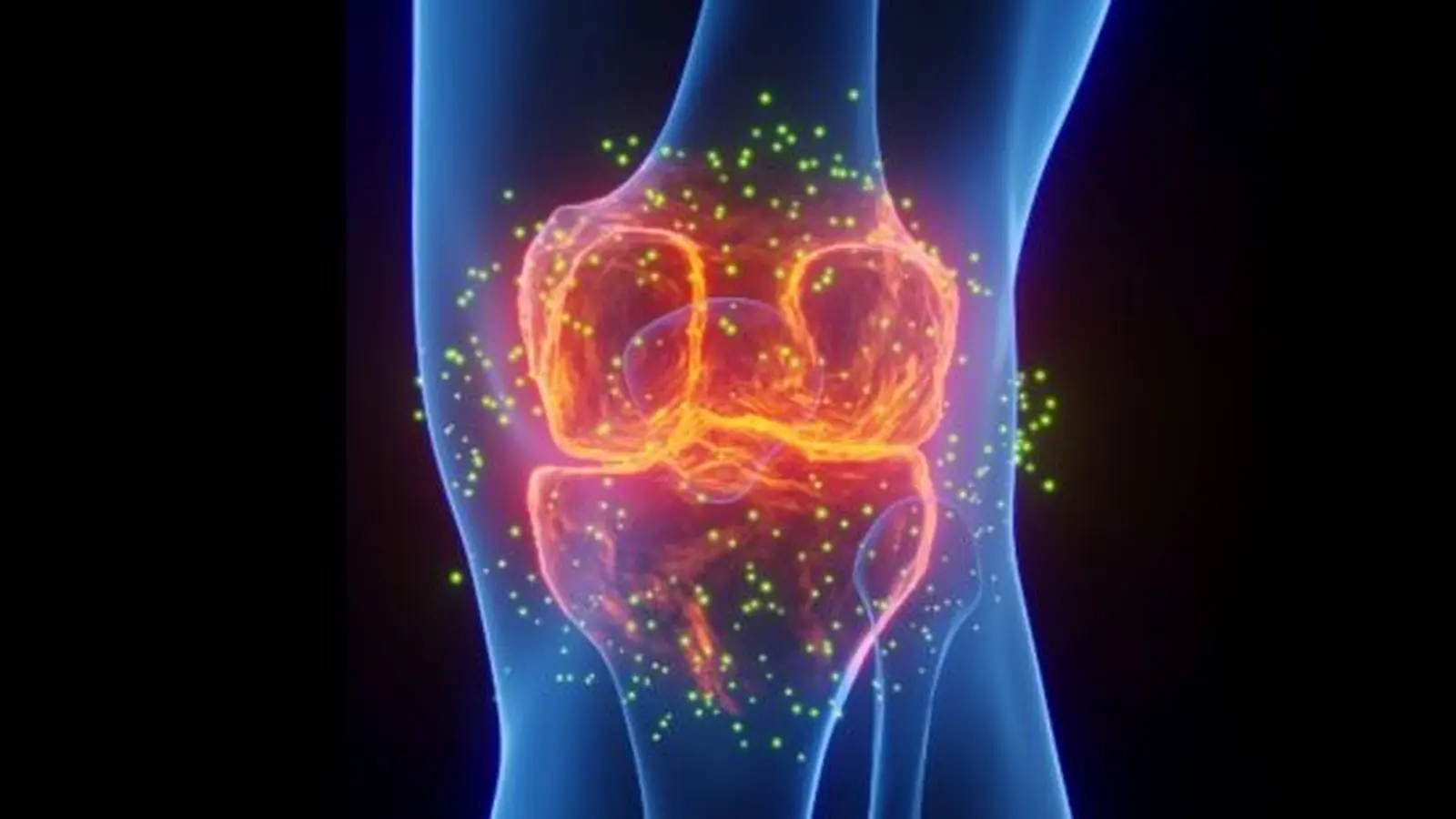
Osteoarthritis impacts the whole joint region
Mechanisms beyond mechanics: inflammation and metabolism
Obesity increases osteoarthritis risk not only by placing extra mechanical load on joints but also by raising levels of inflammatory molecules in the blood and joint tissues. These molecules can accelerate cartilage breakdown and alter pain signalling. Regular physical activity lowers pro-inflammatory markers, reduces oxidative cell damage and can even influence gene expression patterns associated with tissue repair and resilience.
Because exercise has systemic benefits, it simultaneously addresses comorbid conditions common in people with osteoarthritis — for example, type 2 diabetes, cardiovascular disease and depression — improving overall health while targeting the joint disease.
Clinical implications: try exercise before surgery
There are currently no widely available disease-modifying drugs for osteoarthritis. Joint replacement surgery can transform quality of life for patients with advanced disease, but it is major surgery with risks and variable long-term outcomes. For most patients, guideline-based care recommends starting with conservative therapies: structured exercise, weight management where relevant, education and targeted physiotherapy.
Exercise should be introduced early, tailored to the individual’s capacity and continued across all stages of disease. Compared with many pharmacological options, exercise carries far fewer adverse effects and delivers broad health dividends.
Implementation barriers and opportunities
Why, then, is exercise under-prescribed? Barriers include limited time in primary care consultations, insufficient clinician training in exercise prescription, patient beliefs that activity will worsen joint damage, and uneven access to supervised physiotherapy. Addressing these gaps calls for better education of clinicians and patients, wider availability of evidence-based group programs (like GLA:D®), digital platforms for remote exercise supervision, and health-policy incentives to prioritise conservative care before surgery.
Related technologies — wearable sensors, tele-rehabilitation platforms and app-based exercise modules — make it easier to personalise load progression and monitor adherence, offering scalable ways to deliver high-quality exercise interventions to larger populations.
Expert Insight
"Exercise is the single most underused medicine for osteoarthritis," says Dr. Elena Morris, a clinical physiotherapist and researcher specialising in musculoskeletal rehabilitation. "When we teach patients how to move effectively and prescribe progressive resistance and balance work, we see not only pain reduction but real gains in function and confidence. The challenge is making supervised, evidence-based programs accessible and integrating them into routine primary care pathways."
Conclusion
Osteoarthritis is not simply inevitable wear and tear. It is a multifactorial, whole-joint condition shaped by muscle strength, inflammation, metabolic status and movement history. Regular, targeted exercise addresses many of these drivers at once — nourishing cartilage through load, restoring muscle support, improving neuromuscular control and reducing systemic inflammation. For most patients, exercise-based therapy should be the first-line treatment and continued throughout the disease course, with surgery reserved for cases that do not respond to comprehensive conservative care. Embedding exercise as standard practice will require clinician training, patient education and wider access to supervised programs, but the potential benefits for individuals and health systems are substantial.
Source: sciencealert

Leave a Comment